How Knee Arthroscopic Surgery Will Improve Your Quality of Life.
Arthroscopy is a minimally-invasive procedure used for the diagnosis and treatment of conditions affecting joints. Knee Arthroscopic Surgery allows doctors to view the knee joint without making a large incision (cut) through the skin and other soft tissues. Arthroscopy is used to diagnose and treat a wide range of knee problems. Originally, arthroscopy was used mainly for planning a standard open surgery. However, because of the development of new instruments and advanced surgical techniques, many conditions can also be treated using an arthroscope.
Table of ContentsToggle Table of ContentToggle
What is an arthroscope?
An arthroscope is a small tube that is inserted into the body to look inside a joint. It contains a system of lenses, a small video camera, and a light for viewing. The camera is connected to a monitoring system that let a surgeon view the operation while it is being done. The arthroscope is often used with other tools that are inserted through another incision. These tools, unlike the arthroscope, are used for grasping, cutting, and probing.
What is arthroscopy?
Arthroscopy is a minimally-invasive procedure used for the diagnosis and treatment of conditions affecting joints. Originally, arthroscopy was used mainly for planning a standard open surgery. However, because of the development of new instruments and advanced surgical techniques, many conditions can also be treated using an arthroscope.
The joint most frequently examined using arthroscopy is the knee. However, arthroscopy can be used to examine other joints, including the following:
- Shoulder
- Elbow
- Ankle
- Hip
- Wrist
Reasons for the Knee Arthroscopic Surgery
Arthroscopy may be recommended for these knee problems:
- Torn meniscus. Meniscus is cartilage that cushions the space between the bones in the knee. Surgery is done to repair or remove it.
- Torn or damaged anterior cruciate ligament (ACL) or posterior cruciate ligament (PCL)
- Torn or damaged collateral ligament
- Swollen (inflamed) or damaged lining of the joint. This lining is called the synovium.
- Kneecap (patella) that is out of position (misalignment).
- Small pieces of broken cartilage in the knee joint/li>
- Removal of Baker’s cyst. This is a swelling behind the knee that is filled with fluid. Sometimes the problem occurs when there is swelling and pain (inflammation) from other causes, like arthritis<./li>
- Repair of defect in cartilage/li>
- Some fractures of the bones of the knee
During the Knee Arthroscopic Surgery
Arthroscopy may be performed on an outpatient basis or as part of your stay in a hospital. Procedures may vary depending on your condition and your doctor’s practices.
Arthroscopy may be performed while you are asleep under general anesthesia, or while you are awake under localized anesthesia. The type of anesthesia will depend upon the specific procedure being performed. Your anesthesiologist will discuss this with you in advance.
Generally, an arthroscopic procedure follows this process:
- You will be asked to remove clothing and will be given a gown to wear.
- An intravenous (IV) line may be started in your arm or hand.
- If there is excessive hair at the surgical site, it may be clipped off.
- You will be positioned on an operating table, in a manner that provides the best access to the joint being operated on.
- The anesthesiologist will continuously monitor your heart rate, blood pressure, breathing, and blood oxygen level during the surgery.
- The skin over the surgical site will be cleansed with an antiseptic solution.
- The doctor may drain blood from the surgical area by elevating the extremity and/or applying an elastic wrap to the extremity. The doctor may instill a fluid solution (generally a saline solution) before the arthroscope is inserted to help distend the joint and reduce swelling.
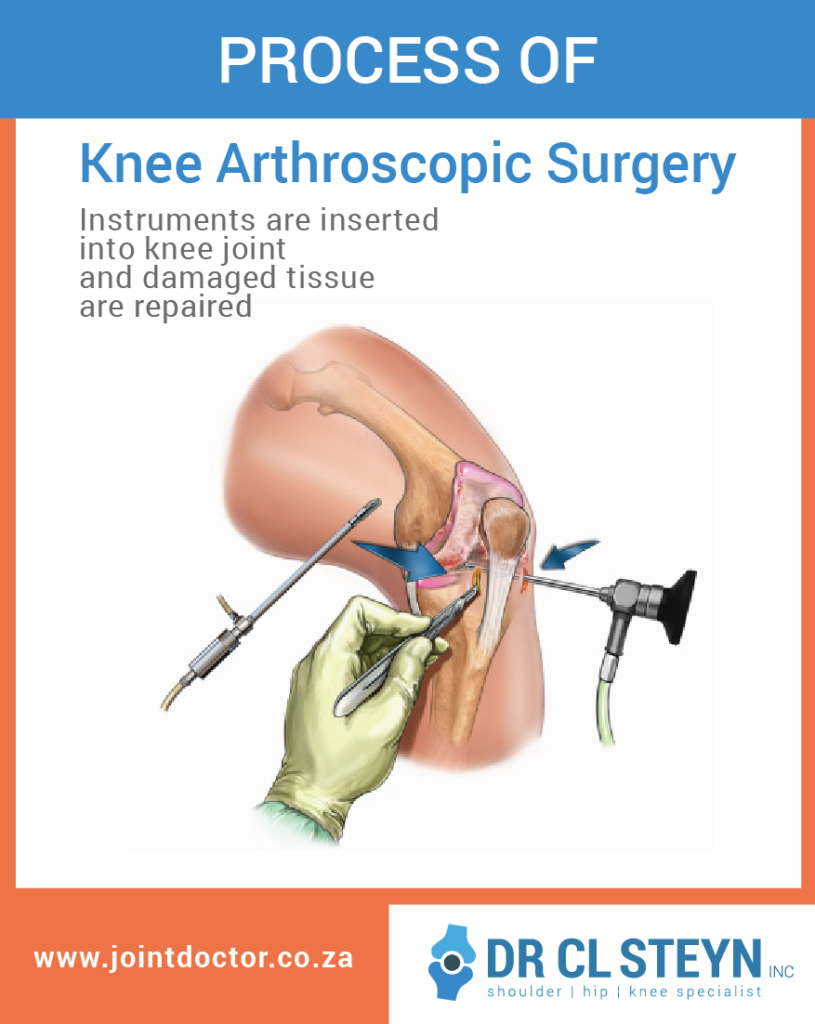
- The doctor will make an incision in the joint area.
- The arthroscope will be inserted through the incision, into the joint.
- Light is transmitted via fiber optics at the end of the arthroscope.
- Corrective surgery, if necessary, may be performed.
- The incision will be closed with stitches or adhesive strips.
- A sterile bandage or dressing will be applied.
Other incisions may be made to introduce other small grasping, probing, or cutting tools.
Information about the interior of the joint is transmitted to a screen.
Knee Arthroscopic Surgery Teaching Video
Risks of the procedure
As with any surgical procedure, complications can occur. Some possible complications may include, but are not limited to, the following:
- Bleeding
- Infection
- Blood clots in the legs or lungs
There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your doctor prior to the procedure.
Before Your Knee Arthroscopic Surgery
Your doctor will explain the procedure to you and offer you the opportunity to ask any questions that you might have about the procedure.
You will be asked to sign a consent form that gives your permission to do the procedure. Read the form carefully and ask questions if something is not clear.
In addition to a complete medical history, your doctor may perform a complete physical examination to ensure you are in good health before undergoing the procedure. You may undergo blood tests or other diagnostic tests.
Notify your doctor if you are sensitive to or are allergic to any medications, latex, tape, and anaesthetic agents (local and general).
Notify your doctor of all medications (prescribed and over-the-counter) and herbal supplements that you are taking.
Notify your doctor if you have a history of bleeding disorders or if you are taking any anticoagulant (blood-thinning) medications, aspirin, or other medications that affect blood clotting. It may be necessary for you to stop these medications prior to the procedure.
If you are pregnant or suspect that you are pregnant, you should notify your doctor.
You will be asked to fast for six hours before the procedure, generally after midnight.
You may receive a sedative prior to the procedure to help you relax. Because the sedative may make you drowsy, you will need to arrange for someone to drive you home.
Based on your medical condition, your doctor may request other specific preparation.
After the Knee Arthroscopic Surgery
After your Knee Arthroscopic Surgery, you will be taken to the recovery room for observation. Your recovery process will vary depending on the type of anesthesia that is given. The circulation and sensation of the affected extremity will be monitored. Once your blood pressure, pulse, and breathing are stable and you are alert, you will be taken to your hospital room or discharged to your home. Arthroscopic surgery is usually done on an outpatient basis.
Once you are home, it is important to keep the incision site clean and dry. Your doctor will give you specific bathing instructions. If stitches are used, they will be removed during a follow-up office visit. If adhesive strips are used, they should be kept dry and generally will fall off within a few days.
Take a pain reliever for soreness as recommended by your doctor. Aspirin or certain other pain medications may increase the chance of bleeding. Be sure to take only recommended medications.
Activity and the use of the joint may be limited for 24 to 48 hours after a diagnostic arthroscopy. If other procedures are performed, such as a ligament repair, your activity and use of your joint may be limited for a longer period of time. Your doctor will give you specific instructions. For knee surgery, you may be given an immobilizer to wear. Your doctor may also instruct you to apply ice to the surgical site and to elevate the knee when sitting. Specific instructions will depend on the exact procedure performed.
Notify your doctor to report any of the following:
- Fever
- Redness, swelling, bleeding, or other drainage from the incision site
- Increased pain around the incision site
- Numbness and/or tingling in the affected extremity
You may resume your normal diet unless your doctor advises you differently. Your doctor may give you additional or alternate instructions after the procedure, depending on your particular situation.
